Dr.Seckin’s Endometriosis Books

Dr. Seckin is a world-renowned, advanced gynecologic surgeon in the world-class treatment of endometriosis excision surgery
How to Manage Endometriosis Nonsurgically
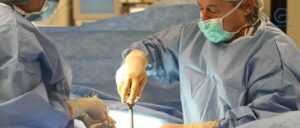
Read about ways to manage endometriosis nonsurgically like medical suppression, painkillers, diet and nutrition, and alternative therapies
Shoulder Pain After Endometriosis Surgery

Read about why you may feel shoulder pain after endometriosis surgery and ways to manage it as well as our unique approach to minimize it.
Was My Endometriosis Surgery Unsuccessful?
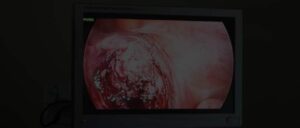
This article is about why endometriosis surgery may be unsuccessful in certain instances and ways in which this can be avoided.
Why Can Endometriosis Return After Surgery?

Read about the factors that may increase the risk of endometriosis recurrence following surgery and how these risks can be minimized.
When is Endometriosis Surgery an Emergency?
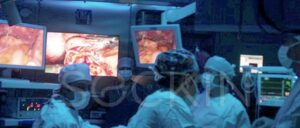
This article is about endometriosis surgery and cases in which it would be considered an emergency approach to treat the disease.
Dr. Tamer Seckin’s Endometriosis Surgery Photos and Videos

Dr. Tamer Seckin on surgical management of endometriosis involving the urinary system with an anterior cul-de-sac endometrioma
Questions to Ask Your Doctor

This article contains a list of questions you might want to ask your surgeon about endometriosis surgery before the procedure.
Endometriosis Videos

Dr. Seckin works with patients to understand symptoms, diagnosis, and the best treatment options for endometriosis.